“Professionalism” has different meanings for different people in different contexts. Kuczewski [1] proposed to define it as the norms of the relationships in which physicians engage in the care of patients. On the other hand, Calman [2] proposed what he called ‘key values’ expected of professional doctors."3
Faculty, fellows and residents have a responsibility to model professionalism for medical students or any peer or junior learners. They should reflect on their own potential for bias in addressing particular students, issues, patients or clinical situations.
The medical education literature suggests that medical schools4:
- Establish clear expectations for professional behavior
- Formally assess professional behaviors
- Provide opportunities for remediating unprofessional behaviors
- Engage in activities that can assist in preventing unprofessional behaviors
- Cultivate a culture of ethical and professional responsibility.
 In cultivating a culture of responsibility, faculty should reflect on and address the "hidden curriculum", issues of cultural, gender or other bias, common misconceptions or assumptions about what it means to be professional or ethical, and the implications of practicing under another physician's license until medical students earn their own. One framework for teaching medical ethics may apply as well to teaching professionalism as professional responsibility.
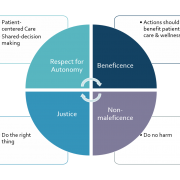
In cultivating a culture of responsibility, faculty should reflect on and address the "hidden curriculum", issues of cultural, gender or other bias, common misconceptions or assumptions about what it means to be professional or ethical, and the implications of practicing under another physician's license until medical students earn their own. One framework for teaching medical ethics may apply as well to teaching professionalism as professional responsibility.
- Respect for autonomy
- Beneficence
- Non-maleficence
- Justice
References
- Kuczewski, M.G. Developing competency in professionalism: The potential and the pitfalls. Bulletin of the ACGME. (October 2001) 3–6.
- Calman, K. The profession of medicine. BMJ. 1994; 309:1140–1143. [PMC free article] [PubMed]
- Altirkawi K. (2014). Teaching professionalism in medicine: what, why and how?. Sudanese journal of paediatrics, 14(1), 31–38.
- Kirk LM. Professionalism in medicine: definitions and considerations for teaching. Proc Bayl Univ Med Cent 2007; 20:13–16. [PMC free article] [PubMed]
Related Resources
Journal of Medical Ethics Google ScholarOn Medical Ethics Ebola & Bioethics

